Dr. Digital
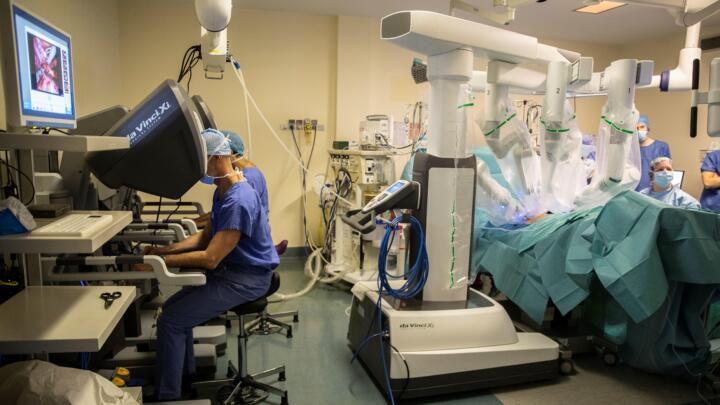
Teamwork in the OR: robots assisting surgeons
Dr. Robot is gaining traction in operating rooms. To date, more than six million robot-assisted surgical procedures have been performed worldwide. The emphasis here is on “assisted” because a robot doesn’t think or control anything but merely carries out the commands issued by a surgeon sitting at a console away from the operating table and using a joystick to steer the robot’s arms. One of the arms guides a 3D camera whose images display the surgical field with tenfold magnification. Due to exact mathematical scaling, the surgeon’s movements are not just transmitted but executed with three times higher precision. Even a potential tremor of the surgeon’s hands is filtered out. Currently, there’s just one surgical robotic system on the market: da Vinci made by Intuitive Surgical, an American company based in California. Experienced surgeons can perform nearly any surgical procedure in the pelvic area, the abdomen or the thorax using da Vinci. Obviously, like any surgery, robot-assisted operations require a certain amount of practice. Especially the lack of haptic feedback during the procedure takes some getting used to.
Robots are increasingly finding their way into other areas of healthcare, too. At the university hospital in Aalborg, Denmark, mechanical assistants sort thousands of blood samples per day, robots holding screens in their hands make it possible for quarantined residents in nursing homes to stay in touch with their families using video-based communication (see section on caregiving). In clinics in the Spanish cities of Palma de Mallorca, Barcelona and Madrid robots are planned to perform corona tests. The 100,000-euro systems are able to take and analyze up to 2,400 samples per day.
54 % of people worldwide
are willing to engage with AI and robotics in healthcare.
Source: PwC Germany
Digital consultation
These numbers underscore how corona has accelerated the digital transformation process in the healthcare sector. While in February 2020, 1,700 doctor’s offices in Germany were offering video-based consultation, this number had increased to 25,000 by April, equating to 1,470-percent growth. Europe-wide, interest in video consultation skyrocketed by 1,000 percent just in the month of April. Zava, an online medical services provider based in London and Hamburg, reported a surge in demand as well, stating that the number of telephone and online consultations had gone up by 60 percent in the first few months of corona – reflecting higher growth than in the ten previous years combined.
Source: Telemedicine Report Germany 2020
Zava’s CEO David Meinerz is convinced that, due to the kind of digital consultations offered by his company or competitors such as Teleclinic and Kry, the number of physical visits to doctor’s offices will decline from an average of ten to four or five, at least in Germany. The uncomplicated procedures speak in favor of digital consultation: Patients use an app to directly select the physicians and specialties they need and make an appointment which, due to the significantly longer office hours, will more than likely be easier to get than with a doctor in private practice. Zava, for instance, offers consultation from 6 in the morning to 10 at night and from 8 in the morning to 8 at night on weekends – in German, English and French. These large time windows not only benefit patients but also doctors who prefer flexible working hours and might even introduce resources into the system that are currently untapped such as physicians taking care of their children at home, who may be able to work during specific hours. If patients find it more convenient to obtain an initial online diagnosis, the crowding issue in hospital emergency rooms could be mitigated as well.
Extensive data protection measures (see info box below) and lack of clarity regarding the assumption of costs by health insurance systems have proven to be a hurdle against further high-speed growth of telemedicine. Telemedicine providers are working at full stretch to eliminate both of these obstacles.
Data protection vs. data flow
German Federal Minister of Health Jens Spahn likes to put the dilemma in a nutshell: Data protection, he says, is something for those who are healthy. Conversely, this means that those who are ill would benefit from a largely unbridled flow of data. Because AI-based diagnostics require data of equally high quality as research databases or the developers of medical device technology. Because interlinked medical devices have to be able to exchange data on the Internet of Things. And because effective exchange of data in emergencies can make the difference between life and death. However, precisely this flow of data is not only hampered by decades-old doctor-patient confidentiality but also by an impenetrable jungle of privacy protection laws worldwide, notwithstanding the fact that the protection of personal and medical data is no doubt important.
In a Digital Health Roadmap, the Bertelsmann Foundation points out approaches to potential solutions:
- Standardized electronic patient files as a therapy management platform with controlled access rights.
- An at least countrywide data linkage infrastructure modeled on the Australian Population Health Research Network. The network in Down Under enables the exchange and interlinking of data between data producers and data managers as well as the parties that want to use the data. The latter have to obtain consent from all relevant data managers plus an ethics committee of the network. Linkage IDs ensure that an individual’s data can be linked in a pseudonomized form but that no third party has access to personal information.
- Enabling voluntary data donations.
- A coherent legal framework providing access to routine data as well as to other anonomized or pseudonomized data of the healthcare system to parties that have a socially relevant interest in using such data.

Organs from a 3D printer
Hardly anyone is astonished anymore about spare parts for cars and household appliances being produced by 3D printers. Also known as additive manufacturing in industrial environments, the digital technology enables the production of personalized, individual aids and products, extending from prosthetic devices such as artificial joints and dentures to individualized anatomical models on which surgical teams practice complex procedures. Using a 3D-printed lung tissue model, researchers are able to more effectively determine how the Covid-19 virus acts in the human body. Together with American universities, the digital manufacturing company Carbon 3D has developed a filter that removes excess chemotherapy drugs administered to cancer patients and thus prevents damage to healthy tissue. Thanks to 3D printing, these filters can be individually adapted to any patient.
Even the production of personalized pharmaceuticals has become established practice thanks to additive manufacturing. As early as in 2015, Spritam, a drug used to treat epilepsy, was the first personalized 3D-printed tablet to be marketed, with tablet dosages tuned to suit the personal needs of any patient.
Research scientists are already working on the additive production of organs and parts of organs, enabling bioprinting of the heart, liver and other organs cloned from DNA stem cells. This might put an end to waiting lists for organ transplants.

AI in diagnostics
In various studies, artificial intelligence has already achieved success rates equating to – or even surpassing – those of experienced physicians. In a pilot study conducted by the University of California, AI detected early stages of Alzheimer’s disease based on brain scans with a 100-percent success rate, even six years on average before the actual diagnosis. In an international study in 2018, 58 dermatologists were pitted against an AI system in the field of skin cancer detection. The physicians achieved a success rate of 86.6 percent while the AI scored 95 percent. Researchers at New York’s Mount Sinai School of Medicine developed a method using natural speech analysis to predict the onset of psychosis in at-risk youths within the next two years. The AI diagnoses presented in January 2018 achieved a success rate of 83 percent. Compared to humans, AI has the advantage of being able to analyze complex data in a matter of seconds, plus, unlike the human brain, AI neither gets tired nor is prone to distraction.
Research projects have also shown that AI is able to deliver diagnoses earlier and with greater precision than established methods in some cases, plus this know-how can be cost-efficiently used anywhere in the world. AI can be involved in the analysis stage of pharmaceutical developments and thus save a lot of development time and, ultimately, costs. The business consultancy PwC estimates the savings potential due to AI just in the areas of dementia, obesity and breast cancer in the next ten years to amount to 172 billion euros, even though the development of artificial intelligence in diagnostics is still in its infancy. The more complex the systems become, the more effectively various data sources (CT, MRT, DNA analysis and cell research, patient data and even hand-written files) can be combined for the assessment of a disease. While the medical profession is going to lose its monopoly of knowledge due to AI, it won’t lose its importance in general. AI will assist physicians in the diagnostic process in that the system proposes a diagnosis based on its experience. However, the attending physician will continue to be indispensable for checking, confirming or, as the case may be, rejecting the AI’s hypothesis as well as for the therapy.
IoT in medicine
Medicine has long recognized the benefits of the Internet of Things for its purposes as well and is developing more and more applications. This field of Industry 4.0 is referred to as Healthcare 4.0. Diabetics, cardiovascular or dialysis patients – like many other chronically ill people – depend on constant monitoring of individual physical parameters and functions: a medical form of condition monitoring for which interlinked devices are tailor-made. Remote therapies and diagnoses are enabled as well, which is ideal for emergency patients and those living in remote areas. In February 2020, Chinese doctors at the hospital in Zhejiang controlled an ultrasonic examination in Wuhan – 700 kilometers away from Zhejang and a locked-down corona hotspot at the time – via a 5G high-speed data network. Due to the high transmission rates of the new mobile telecommunications technology, the physicians were able to look at the huge data volumes of the images almost in real time.
Robotics in rehabilitation
As early as in the 1990s, therapists used robotics to assist them in their work, which makes them members of the group of pioneers in healthcare. By now, a wide variety of robots are used in rehabilitation worldwide for training patients to walk, move their arms or speak again after having suffered neural damage. Like in surgery or in diagnostics, robots assist and ease the workload of healthcare professionals, but do not replace them. Science has confirmed that intensity, repetition and an early beginning of rehabilitation massively increase the chances of recovery. Untiring and always ready robots can be of great help in this context. By recording specific training parameters such as the number of steps, force exerted or coordination of movements, the machine can provide direct feedback which can have a motivating effect.
Robotics in caregiving
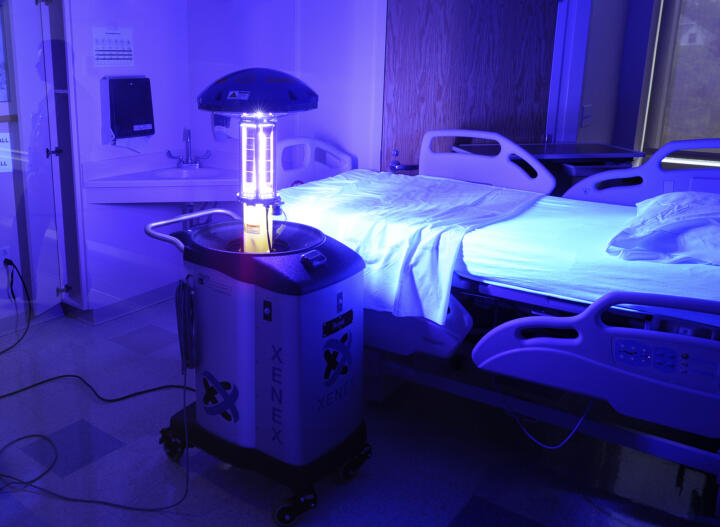
As life expectancy keeps growing so does the need for delivering care to the elderly. But even at this juncture, there’s a shortage of nursing staff – and the shortfall keeps increasing. In 2030, there’ll be a shortage of 500,000 nurses in Germany alone, according to a study by the Bertelsmann Foundation, and nearly 400,000 in Japan, according to government estimates there. Robots might provide a remedy, offering a wide range of possible uses, from so-called exoskeletons assisting nurses in lifting patients and machines delivering meals, beverages or laundry. During the corona pandemic, Chinese hospitals ordered 2,000 disinfection robots from the Danish manufacturer Blue Ocean Robotics. There are robots that demonstrate gymnastics exercises and socially-assistive humanoid robots which, through their interaction with patients, are able to compensate for lacking social contacts and – as strange as that may sound – even for human affection and warmth. The robotic seal Paro with big round eyes and a fluffy white fur is a global bestseller of this robotic species. More than 4,000 of these therapeutic animals that cost 5,000 euros are in interactive use worldwide with cancer patients, autistic children or Alzheimer patients. The high purchasing costs of these machines are contrasted by a number of key benefits: robots can be used around the clock, they don’t get sick, and they don’t go on vacation.
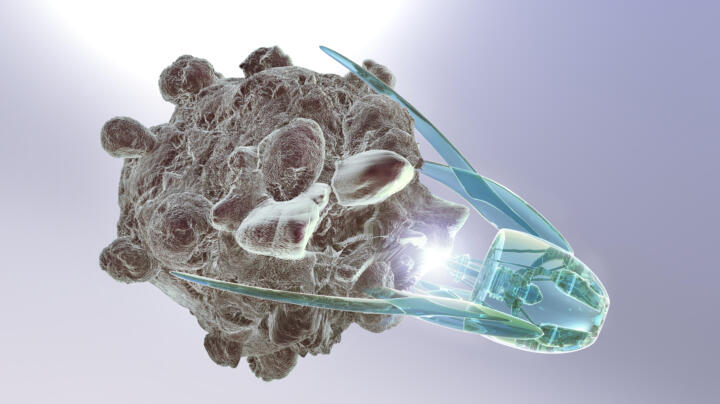
Nanorobots glide through the body
In 1966, a team of research scientists shrunk itself to virus size and navigated a human body on board of a micro-submarine – at least in the science fiction movie “Fantastic Voyage.” While we’re still far away from shrinking physicians, doctors have in fact successfully maneuvered the first tiny nano-robots through human vascular systems. The propeller that drives them is 200 times smaller than the diameter of a human hair. The distant aim of this high-tech medicine is to enable surgery in parts of the body that are difficult to access or the conveyance of medicines with pinpoint accuracy, thus reducing side effects. In experiments with mice, the deployment of nanobots has already successfully fought tumors and metastases. Consequently, the medical profession is pinning huge hopes on these tiny devices.
In the interest of health

Schaeffler provides to its employees at German locations an extensive health portal, the “Schaeffler Health Coach.” The company’s health management team is able to reach all Schaeffler employees via this portal that can be used as both an app and a desktop version. All health-promoting programs, which employees can freely choose from, can be viewed in the Schaeffler Health Coach. In addition, updates on health-related topics and tips are uploaded at regular intervals. The tool has been active since the end of 2018 and was extended by the important factor of telemedicine in April 2019. As a result, employees are able to receive medical advice around the clock.